

New South Wales’ State Insurance Regulatory Authority (SIRA) has outlined a two‑year program to change how it regulates health providers in the state’s personal injury schemes, following an independent strategic review led by Sue Dawson. The Health Provider Regulation Implementation Roadmap, released after Dawson’s review, sets out a staged approach to altering SIRA’s regulatory framework across workers’ compensation and compulsory third party (CTP) insurance.
SIRA has accepted the review’s findings and has committed to work through the roadmap’s directions, actions, and time frames. The review states that “effective regulation of health providers is central to the ability of the personal injury schemes to meet the objective of recovery for injured persons” and notes that the annual cost of health services within the schemes is now above $1.8 billion. SIRA plans to report quarterly on progress, with updates to be published on its website.
According to SIRA, the strategic review was conducted in four phases between August 2025 and March 2026, combining research, cross‑government consultation, and targeted engagement with stakeholders. The first phase, from August to October 2025, focused on research and scoping. In November and December 2025, a draft discussion paper was prepared and refined through consultation with government agencies. A public discussion paper was then released in January and February 2026 for targeted consultation, resulting in 17 consultation meetings and 29 written submissions from stakeholders including insurers and health provider representatives. Reform options and implementation actions were finalised in March 2026, when Dawson presented the roadmap.
The review highlights four main areas of concern in the existing arrangements:
The report records stakeholder feedback that health providers “are already heavily regulated” and that a lack of clarity about SIRA’s additional role “creates confusion and undue administrative burden.” It also points to more than 40 regulatory and policy instruments governing provider obligations, many of which were assessed as not directly contributing to improvements in service quality.
The first strategic direction in the roadmap is to clarify and document the respective roles of SIRA and specialist health regulators in relation to health providers working in the NSW personal injury schemes. Under the proposed arrangements, health profession regulators are to retain responsibility for clinical performance and professional misconduct issues, while SIRA is to focus on scheme‑related matters such as reporting quality, billing approvals and administrative compliance, overservicing, low‑value care, and provider business practices.
Planned actions include a tripartite memorandum of understanding between SIRA, the Health Care Complaints Commission (HCCC), and the Health Professional Councils Authority (HPCA) to support information exchange, joint communications, and ongoing oversight of emerging risks. SIRA will also review its memorandum of understanding with the Independent Review Office (IRO) and work with Commonwealth entities, including the National Disability Insurance Agency (NDIA), on fraud detection and enforcement linked to scheme services.
In addition, SIRA is to work with the Australian Health Practitioner Regulation Agency (Ahpra) to align professional standards where they intersect with personal injury schemes. An initial focus area is guidance on medico‑legal assessments and reporting, including requirements “to be clinically sound,” to “link diagnosis, treatment, and functional capacity,” and “to tailor reasoning to individual circumstances without formulaic reporting.”
The second direction focuses on regulatory design. SIRA proposes to adopt a graduated, risk‑based model under which core obligations apply to all health providers delivering services under the schemes, with additional obligations for functions assessed as higher risk or of heightened importance to scheme objectives.
Early work under this direction includes:
The roadmap also calls for a review of fee and servicing parameters in the context of scheme sustainability. Areas flagged include reliance on Australian Medical Association (AMA) and Medicare Benefits Schedule (MBS) rates, exemptions from pre‑approval, and the operation of fee orders and pre‑approval thresholds in the CTP scheme.
The third direction addresses how SIRA will use risk information in supervising health providers and enforcing scheme rules. SIRA plans to establish standardised business processes for triaging complaints and other regulatory information about providers. Complaints are to be handled under a single process designed to identify and prioritise apparent and potential risks. Significant fraud allegations will be referred to a dedicated fraud function, while other inputs will be analysed to flag issues for regulatory action. SIRA has said that these processes will be documented and made public.
A risk assessment framework, based on categories and indicators developed through the review, will guide compliance and enforcement decision‑making. To support this, SIRA intends to set up a data and analytics program drawing on internal and external data, with routine reporting on risk indicators and complaints trends. The roadmap refers to ongoing work, through the Department of Customer Service, on an artificial intelligence tool to analyse Personal Injury Commission (PIC) decisions to identify providers presenting higher risk.
Oversight of these activities is to include a Quarterly Planning and Review Strategy Meeting chaired by SIRA’s executive director of regulatory operations. The meeting will review the volume and focus of regulatory activity, performance against expected outcomes, and systemic patterns emerging from intelligence, as well as issues raised by insurers, providers, and peak bodies. Immediate compliance focus areas listed in the roadmap include provider billing (covering fee levels, duplication, and referral patterns linked to sustained treatment volumes) and insurer payment timeliness, which the review notes has been raised as a factor in provider disengagement from the schemes. SIRA will also implement case planning and performance monitoring tools, including key performance indicators, case allocation and dashboard reporting, system alerts for high‑risk matters, and templates for regulatory action. A quarterly public report on performance against KPIs and significant compliance and enforcement activity is to be introduced.
The fourth direction is aimed at establishing more consistent engagement with health providers and insurers and improving understanding of scheme obligations. Under the roadmap, SIRA’s Health Supervision team will nominate a health provider liaison officer as a single point of contact for provider regulatory issues. SIRA will convene quarterly bilateral forums with health provider peak bodies and with insurers, with senior representation and agreed processes for tracking and reporting on actions.
These forums will receive a quarterly Health Provider Regulatory Activity and Performance Briefing, which SIRA also intends to publish to outline risk and compliance patterns and current areas of regulatory focus. SIRA will work with the Health Professional Councils Authority (HPCA) to use existing health provider bulletins to reach providers and will establish an annual tripartite forum bringing together provider peaks and insurers to discuss issues at the interface between provider operations and insurer decision‑making.
On education, the roadmap proposes expanded training and information programs co‑designed with provider peaks and linked to existing offerings such as those from the Personal Injury Education Foundation and Monash University’s compensable health and medicine course. Training is to address the schemes’ functional capacity improvement objectives, high‑value care, and scheme sustainability. The document also identifies specific actions within the workers’ compensation reform program to support insurer and provider understanding and application of the “reasonable and necessary” test.
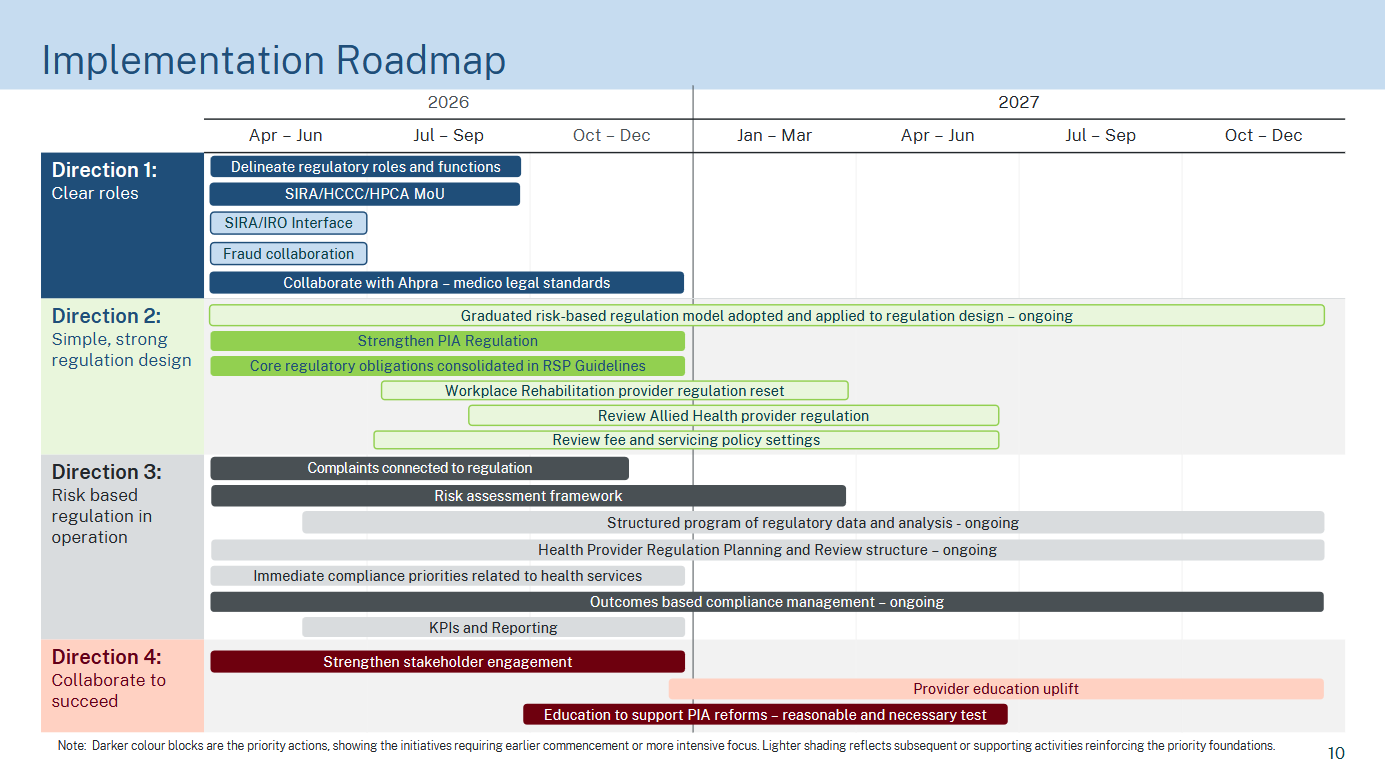
The roadmap describes the reform agenda as a “foundational transformation” requiring sustained work over one to two years, with sequencing intended to deliver some early changes while longer‑term system reforms are developed and implemented. Initial priorities over the first three to six months include changes to regulatory design for permanent impairment assessors and relevant service providers, clarification and communication of regulatory roles and medico‑legal reporting expectations, implementation of new complaints and risk assessment processes, and re‑establishment of structured stakeholder engagement and education. The review states that, with these actions in place, people with an injury “will have increased confidence that they will receive health services that are reasonable and necessary to assist them to return to work or life activities” and that there will be a stronger focus on the sustainability of NSW personal injury schemes for future injured people.
